The logic of medical language
In this chapter, we will discuss the current medical language. Specifically, we will discuss the study of the relationships between linguistic expressions and the world to which they refer, or which they should describe.
The conclusion is that once the vagueness and ambiguity of this form of language (and therefore the negative consequences that all this entails) have been revealed, there is a need to make it more precise and complete. We want to focus on more mathematical and rigorous reasoning because it can be much more effective if we can manipulate it the right way as we will discuss in this chapter.
Medical language is an extended natural language
Language is a source of misunderstandings and errors and in medicine: actually, often the language we use leaves us in trouble because it is semantically underdeveloped and does not agree with standard scientific ideas. To better explain this concept, which apparently seems off-topic, we must describe some essential characteristics of the logic of language that will make us better understand why a term like orofacial pain can take on a different meaning following a classical logic or a formal one.
The passage from classical logic to formal logic does not imply adding a minor detail as it requires an accurate description. Although medical and dental technology has developed breathtaking models and devices in many dentistry rehabilitation disciplines, such as electromyographs, cone-beam CT, oral digital scan, etc., the medical language still needs improvement.
First of all, we must distinguish between natural languages (English, German, Italian, etc.) and formal languages, such as mathematics. The natural ones emerge naturally in social communities as much as in scientific communities. Simultaneously, the formal languages are artificially built for use in disciplines such as mathematics, logic and computer programming. Formal languages are characterized by syntax and semantics with precise rules, while a natural language has a fairly vague syntax known as grammar and lacks any explicit semantics.
To keep this study active and engaging, and to avoid it degenerating into a boring treatise on the philosophy of science, let’s consider a very explanatory clinical case. We will deal with it using different languages:
Clinical case and logic of medical language
Patient Mary Poppins (obviously a fictitious name) was followed and treated for over 10 years by multiple colleagues, including dentists, family doctors, neurologists and dermatologists. Her brief story is as follows:
- the woman first noticed small patches of abnormal pigmentation on the right side of her face at the age of 40 (she was now 50).
On her admission to a dermatological division, a skin biopsy was performed, and it was consistent with the diagnosis of localized scleroderma of the face (morphea);
corticosteroids were prescribed. - At the age of 44, she began to have involuntary contractions of the right masseter and temporal muscles; the contractions increased in duration and frequency over the years. The spasmodic contractions were referred to by the patient as both day and night lock.
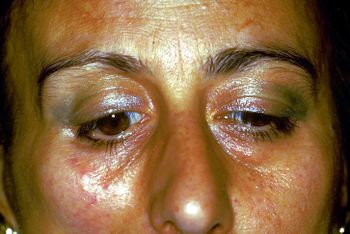
At her first neurological evaluation, dyschromia was less evident. Still, her face was asymmetrical due to a slight indentation of the right cheek and marked hypertrophy of the masseter and right temporal muscles.
The diagnoses were varied, due to the limitation of the medical language as we will see below.
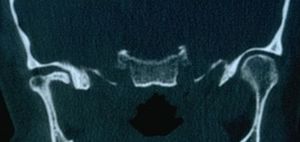
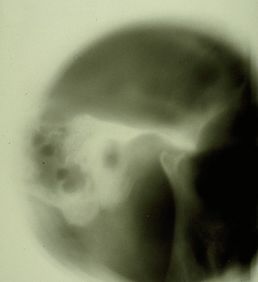
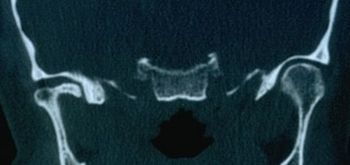
The clinical scenario can be reduced to the following: the patient expresses in her natural language the psychophysical state that has long afflicted her; the dentist, after having performed a series of tests such as anamnesis, a stratigraphy and a CT scan of the TMJ (Figures 1, 2 and 3), concludes with a diagnosis of 'Temporomandibular Disorders', which we call 'TMDs'[1][2][3]; the neurologist remains instead on a diagnosis of organic neuromotor pathology of the 'neuropathic Orofacial Pain' (nOP) type, excluding the TMDs component, or does not consider the main cause. To not sympathize with either the dentist or the neurologist in this context, we will consider the patient suffering from ‘TMDs/nOP’; so nobody fights.
«But who will be right?»
|
We are obviously in front of a series of topics that deserve adequate discussion because they concern clinical diagnostics.
Unlike the formal languages of mathematics, logic and computer programming (which are artificial systems of signs with precise rules of syntax and semantics), most scientific languages develop as a simple expansion of natural language with a mix of some technical terms. The medical language belongs to this intermediate category. It emerges from natural and everyday language by adding terms such as 'neuropathic pain', 'Temporomandibular Disorders', 'demyelination', 'allodynia', etc. This is why it has no specific and semantic syntax beyond the one it takes from natural language. For example, let's consider the term 'disease' referring to the patient Mary Poppins: this is a term that indicates the fundamental concept of medicine, disease at the base of nosology and clinical research and practice. It is expected to be a well-defined technical term, yet it is still an indefinite term.
Nobody knows what it means precisely and, apart from some philosophers of medicine, nobody is interested in its exact meaning. For example, does 'disease' concern the subject/patient or the System (as a living organism)? And consequently: can a patient who is not sick in time live together with a system already in a state of structural damage in time ?
The term languishes without any semantics as if it were irrelevant or gratuitous and its derivatives share the same semantic obscurity with it.[4]
- In short,
- is the patient Mary Poppins sick, or is the chewing System damaged?
- Is it instead a 'System' disease considering the masticatory System in its entirety consisting of subsets such as receptors, peripheral and central nervous tissue, maxillary bones, teeth, tongue, skin, etc.,?
- Or, is it an 'organ' disease involving in this specific case the temporomandibular joint (TMJ)?
These brief notes demonstrate how the inaccuracies and peculiarities of natural language enter medicine through its syntactic and semantically underdeveloped form. We should deal with some of these peculiarities with concrete clinical examples.
Clinical approach
(hover over the images)
What does a medical term mean
Let us ask ourselves what "meaning" means.
The Cambridge Dictionary says that "The meaning of something is what it expresses or represents"[5]. As simple as it may seem, the notion of "meaning" is rather generic and vague; there is still no commonly accepted answer to the question 'what does "meaning" mean?' Controversial theories of meaning have been advanced, and each has its advantages and shortcomings[6][7].
Traditionally, a term is displayed as a linguistic label meaning an object in a world, concrete or abstract. The term is thought to stand in the language as a representative for that object, e.g. ‘apple’ for the famous fruit. This term ‘apple’ will have the same meaning for the American child, the European adult or the Chinese elder, while the meaning ‘Orofacial Pain’ will have an intention for the neurologist, one for the dentist, and its own essence the unfortunate Mary Poppins.
Such expressions do not derive their meaning from representing something in the world out there, but how they relate to other terms within one’s world or context.
The meaning of pain for Mary Poppins is concerning what it can mean to her, to her conscience, and not about the external world: actually, asking the patient to attribute a numerical value to his pain, say from 0 to 10, makes no sense, has no meaning, because there isn't any internal normalizing reference to one's world or context.
The same is true for the neurologist who will give sense to the term 'pain in the right half face' solely in his/her context based on synapses, axons, ion channels, action potentials, neuropeptides etc.
The dentist will do the same, based on his/her context consisting mainly of teeth, temporomandibular joint, masticatory muscles, occlusion etc.
Concepts should not be neglected when it comes to 'differential diagnosis', because they could be sources of clinical errors. For this reason, we should reflect on the modern philosophy of 'Meaning', which began with Gottlob Frege[8], as a compound of "extension" and "intention" of a term that expresses a concept.
The concept has its extension (it includes all beings with the same quality) and 'understanding' (a complex of markers referred to the idea). For example, the concept of pain refers to many human beings, but it is more generic (great extension, but little understanding). If we consider the pain in patients who receive, for example, dental implants, in patients with ongoing inflammatory dental pulpitis and patients with neuropathic pain (atypical odontalgia)[9] we'll have:
- Increases in the mechanical perception threshold and the sensory perception threshold related to C fibres' activation.
- Somatosensory abnormalities such as allodynia, reduced mechanical perception and impaired pain modulation in patients with atypical odontalgia.
- No somatosensory alteration after implant insertion, although patients report mild pain in the treated region.
On ‘pain’ in general we can say that it has a wide extension and minimal understanding, but if we consider the type of pain mentioned above, for example in patients who receive dental implants, in patients with ongoing inflammatory dental pulpitis and in patients with neuropathic pain (atypical odontalgia), it becomes evident that the greater the understanding is, the smaller the extension.
The intension of a concept, on the other hand, is a set of aspects that distinguish it from the others. These are the characteristics that differentiate the generic term of "pain", which by articulating the intension of a concept automatically reduces its extension. Obviously, though, various generality scales can descend from a concept depending on which aspect of its intension is articulated. That is why we could conceptually distinguish pain in the TMJ from neuropathic pain.
We can conveniently say, therefore, that the meaning of a term with respect to a particular language is an ordered couple, consisting of extension and intension, in a world that we will now call ‘context’.
Precisely with reference to the context we must point out that:
- In the dental ‘context’, the term pain in the right half face represents a relatively large extension (so that it can be classified in an area that includes the ‘TMDs’) and an intension composed of a series of clinical characteristics perhaps supported by a series of instrumental radiological investigations, EMG, axiographic etc.
- In the neurological ‘context’, however, the term pain in the right half face represents a relatively wide ‘nOP’ extension and an intension composed of a series of clinical features, perhaps supported by a series of instrumental radiological investigations, EMG, somatosensory evoked potentials, etc.
This brief but essential argument allows us to ascertain how the linguistic expression of a medical language is vulnerable for a series of reasons; among these, please note semantic incompleteness, as well as how a meaning can be so different in different contexts that the terms ‘nOP’ or ' TMDs' become ambiguous with these premises[10].
Ambiguity and Vagueness
As said, beyond the language used, the meaning of a medical term also depends on the contexts from which it originates, and this can generate ‘ambiguity’ or ‘polysemy’ of the terms. A term is called ambiguous or polysemic if it has more than one meaning. Ambiguity and vagueness have been the subject of considerable attention in linguistics and philosophy[11][12][13]; but despite the significant detrimental effect of ambiguity and vagueness on adherence to and implementation of the Clinical Pratice Guideline (CPG)[14], these concepts have not been explored and differentiated yet in a medical context.
Doctors' interpretation of vague terms varies greatly[15], leading to a reduced grip and q greater practice variation from CPGs. Ambiguity is classified into syntactic, semantic and pragmatic types[16].
As previously described, the meaning of a simple linguistic expression referred to by Mary Poppins has at least three different meanings in three different contexts. The ambiguity and vagueness in the linguistic expression behind the term ‘orofacial pain’, which at the same time could be a source of diagnostic errors, mainly concerns the inefficiency of the medical language logic in decrypting the machine message that the System sends in real time to the exterior.
Let's spend a minute trying to describe this interesting topic of encrypted machine language from which the following chapters will be articulated.
Orofacial pain does not have a meaning in its most genuine lexical form, but rather in what it means in the context in which it exists: a whole series of domains referred to and generated by it such as clinical signs, related symptoms and interactions with other neuromotor, trigeminal, dental districts, etc. This machine language does not correspond to verbal language, but to an encrypted language built on its own alphabet, that generates the message to be converted into verbal (natural) language. Now the problem shifts to the language logic used to decrypt the code. In order to describe this concept in an understandable way, let’s contemplate a series of examples.
We are supposing that the unfortunate Mary Poppins is suffering from ‘orofacial pain’, and she is representing the following to the healthcare professionals to whom she relates:During this period, ‘vesicular lesions’ formed on my skin, which were more evident in the right half of my face.
In this period, however, the pain became more intense and intermittent»
The healthcare worker, who may be a dermatologist, a dentist or a neurologist, picks up some verbal messages in Mary Poppins’ dialogue, such as ‘diffuse facial pain’ or ‘TMJ’ or ‘vescicular lesion’, and establishes a series of hypothetical diagnostic conclusions that have nothing to do with the encrypted language.
Here, however, we should abandon a little the acquired patterns and opinions to better follow the concept of ‘encrypted language’. Let's suppose, therefore, that the System is generating and sending the following encrypted message, for instance: Ephaptic.
Now, what has ‘Ephaptic’ to do with nOP or TMDs?
Nothing and everything, as we will better verify at the end of the chapters about the logic of medical language; but by now we will dedicate some time to the concepts of encryption and decryption. We have perhaps heard about them in spy movies or in information security, but they are important in medicine too, you'll see.
Encryption
Let us continue with our example:
Let us take a common encryption and decryption platform. In the following example we will report the results of an Italian platform but we can choose any platform because the results conceptually do not change:
You type your message in plain text, the machine converts it into something unreadable, but anyone knowing the "code" will be able to understand it.
Let us suppose, then, that the same happens when the brain sends a message in its own machine language, made up of wave trains, packets of ionic fields and so on; and that carries a message with it to decrypt the ‘Ephaptic’ code.
This message from the Central Nervous System must first be transduced into verbal language, to allow the patient to give meaning to the linguistic expression and the doctor to interpret the verbal message. In this way, however, the machine message is polluted by the linguistic expression: both by the patient, who is unable to convert the encrypted message with the exact meaning (epistemic vagueness), and by the doctor, because he/she is conditioned by the specific context of his/her specialization.
The patient, actually, by reporting a symptomatology of orofacial pain in the region of the temporoandibular joint, virtually combines the set of extension and intention into a diagnostic concept that allows the dentist to formulate the diagnosis of orofacial pain from temporomandibular disorders. (TMDs).
Very often the message remains encrypted at least until the system is damaged to such an extent that clinical signs and symptoms emerge so striking that, obviously, they facilitate the diagnosis.
Understanding how the encryption works is quite simple (go to decryption platform chooses and to try it out):
- choose an encryption key among those selected;
- type a word;
- get a code corresponding to the chosen key and the typed word.
For example, if we insert the word ‘Ephaptic’ in the platform encryption system, we will have an encrypted code in the three different contexts (patient, dentist and neurologist) which correspond to the three different algorithmic keys indicated by the program, for instance: the A key corresponds to the patient's algorithm, the B key to the dental context and the C key to the neurological context.
In the case of the patient, for example, writing Ephaptic and using the A key, the "machine" will give us back a code like
The key can be defined as "Real context".
«Why do you say that the patient's "key" is defined as the REAL one?»
(difficult answer, but please observe the Gate Control phenomenon and you will understand) |
First of all: Only the patient is unconsciously aware of the disease that afflicts his own system, but he does not have the ability to transduce the signal from the machine language to the verbal language. The same procedure occurs in 'Systems Control Theory', in which a dynamic control procedure called ‘State Observer’ is designed to estimate the state of the system from output measurements. Matter of fact, in the control theory, observability is a measure of how much the internal state of a system can be deduced from the knowledge of its external outputs[17]. While in the case of a biological system a ‘Stochastic Observability’ of linear dynamic systemsis preferred[18], the Gramian matrices are used for the stochastic observability of nonlinear systems[19][20].
This would already be enough to bring now our attention on an extraordinarily explanatory phenomenon called Gate Control. If a child gets hit in the leg while playing soccer, in addition to crying, the first thing he does is to rub extensively the painful area so that the pain decreases. The child does not know the ‘Gate Control’, but unconsciously activates an action that, by stimulating the tactile receptors, closes the gate at the entrance of the nociceptive input of the C fibres, consequently decreasing the pain; the phenomenon was discovered only in 1965 by Ronald Melzack and Patrick Wall[21][22][23][24][25].
As much as in computers, encryption-decryption also takes place in biology. In fact, in a recent research the authors examined the influence of molecular mechanisms of the ‘long-term potentiation’ (LTP) phenomenon in the hippocampus on the functional importance of synaptic plasticity for storage of information and the development of neuronal connectivity. It is not yet clear if the activity modifies the strength of the single synapses in a digital (01, all or nothing) or analog (graduated) way. In the study it emerges that individual synapses appear to have an 'all or nothing' enhancement, indicative of highly cooperative processes, but different thresholds for undergoing enhancement. These findings raise the possibility that some forms of synaptic memory may be digitally stored in the brain[26].
Decryption
Now, assuming that the machine language and the assembler code are well structured, we insert the encrypted message from the Mary Poppins System in the 'Mouth of Truth‘[27]:
Let's pretend that we are Martians in possession of the right key (algorithm or context) the A key that corresponds to the 'Real Context'. We would be able to perfectly decrypt the message, as you can verify by entering the code in the appropriate window:
These are extraordinarily interesting elements of language logic, and please note that the encrypted message of the real context ‘meaning’ of the ‘disease’, the A key, is totally different from the one encrypted through the B keys and the C key: they are constructed in conventionally different contexts, while there is only one reality and this indicates a hypothetical diagnostic error.
This means that medical language logics mainly built on an extension of verbal language, are not very efficient in being quick and detailed in diagnostics, especially the differential one. This is because the distortion due to the ambiguity and semantic vagueness of the linguistic expression, called ‘vagueness epistemic’ or ‘epistemic uncertainty’, or better ‘uncertain knowledge’, forcibly directs the diagnosis towards the specialist reference context and not on the exact and real one.«Why, then, are we relatively successful in diagnostics?»
(An entire separate encyclopedia would be needed to answer to this question, but without going too far, let's try to discuss the reasons.) |
Basic diagnostic intuition is a quick, non-analytical and unconscious way of reasoning. A small body of evidence indicates the ubiquity of intuition and its usefulness in generating diagnostic hypotheses and ascertaining the severity of the disease. Little is known about how experienced doctors understand this phenomenon, and about how they work with it in clinical practice. Most reports of the physician’s diagnostic intuition have linked this phenomenon to non-analytical reasoning and have emphasized the importance of experience in developing a reliable sense of intuition that can be used to effectively engage analytical reasoning in order to evaluate the clinical evidence. In a recent study, the authors conclude that clinicians perceive clinical intuition as useful for correcting and advancing diagnoses of both common and rare conditions[28]It should also be noted that the Biological System sends a uniquely integrated encrypted message to the outside, in the sense that each piece of code will have a precise meaning when individually taken, while if combined with all the others it will generate the complete code corresponding to the real message, that is to "Ephaptic”.
This outcome comes from the deletion of the last two elements of the originating code: resulting from . So, part of the code is decrypted (Ef) while the rest remains encrypted and the conclusion speaks for itself: it is not enough to identify a series of specific tests, yet it is necessary to know how to tie them together in a specific way in order to complete the real concept and build the diagnosis.
Therefore, there is a need for:«A System Logic that integrates the sequence of the machine language code»
(true! we'll get there with a little patience) |
Final Considerations
The logic of language is by no means a topic for philosophers and pedagogues; but it substantially concerns a fundamental aspect of medicine that is Diagnosis. Note that the International Classification of Diseases, 9th Revision (ICD-9), has 6,969 disease codes, while there are 12,420 in ICD-10 (OMS 2013)[29]. Based on the results of large series of autopsies, Leape, Berwick and Bates (2002a) estimated that diagnostic errors caused 40,000 to 80,000 deaths annually[30]. Additionally, in a recent survey of over 6,000 doctors, 96% believed that diagnostic errors were preventable[31].
Charles Sanders Peirce (1839–1914) was a logician and practicing scientist[32]; he gradually developed a triadic account of the logic of inquiry. He also distinguishes between three forms of argumentation, types of inference and research methods that are involved in scientific inquiry, namely:
- Abduction or the generation of hypotheses
- Deduction or drawing of consequences from hypotheses; and
- Induction or hypothesis testing.
In the final part of the study conducted by Donald E Stanley and Daniel G Campos, the Peircean logic is considered as an aid to guaranteeing the effectiveness of the diagnostic passage from populations to individuals. A diagnosis focuses on the individual signs and symptoms of a disease. This manifestation cannot be extrapolated from the general population, except for a very broad experiential sense, and it is this sense of experience that provides clinical insight, strengthens the instinct to interpret perceptions, and grounds the competence that allows us to act. We acquire basic knowledge and validate experience in order to transfer our observations into the diagnosis.
In another recent study, author Pat Croskerry proposes the so-called "Adaptive Expertise in Medical Decision Making", in which a more effective clinical decision could be achieved through adaptive reasoning, leading to advanced levels of competence and mastery[33].
Adaptive competencies can be obtained by emphasizing the additional features of the reasoning process:
- Be aware of the inhibitors and facilitators of rationality (Specialists are unwittingly projected towards their own scientific and clinical context).
- Pursue the standards of critical thinking. (In the specialist, self-referentiality is supported and criticisms from other scientific disciplines or from other medical specialists are hardly accepted).
- Develop a global awareness of cognitive and affective biases and learn how to mitigate them. Use argument that reinforces point 1.
- Develop a similar depth and understanding of logic and its errors by involving metacognitive processes such as reflection and awareness. Topic is already mentioned in the first chapter ‘Introduction’.
In this context, extraordinarily interesting factors emerge that lead us to a synthesis of all what has been presented in this chapter. It is true that the arguments of abduction, deduction and induction streamline the diagnostic process but we still speak of arguments based on a clinical semeiotics, that is on the symptom and/or clinical sign[29]. Even the adaptive experience mentioned by Pat Croskerry is refined and implemented on the diagnosis and on the errors generated by a clinical semeiotics[33].
Therefore, it is necessary to specify that semeiotics and/or the specific value of clinical analysis are not being criticized because these procedures have been extraordinarily innovative in the diagnostics of all time. In the age in which we live, however, it will be due to the change in human life expectancy or the social acceleration that we are experiencing, ‘time’ has become a conditioning factor, not intended as the passing of minutes but essentially as bearer of information.
- In this sense, the type of medical language described above, based on the symptom and on the clinical sign, is unable to anticipate the disease, not because there is no know-how, technology, innovation, etc., but because the right value is not given to the information carried over time
This is not the responsibility of the health worker, nor of the Health Service and nor of the political-industrial class because each of these actors does what it can do with the resources and preparation of the socio-epochal context in which it lives.
The problem, on the other hand, lies in the mindset of mankind that prefers a deterministic reality to a stochastic one. We will discuss these topics in detail.
In the following chapters, all dealing with logic, we will try to shift the attention from the symptom and clinical sign to the encrypted machine language: for the latter, the arguments of the Donald E Stanley-Daniel G Campos duo and Pat Croskerry are welcome, but are to be translated into topic ‘time’ (anticipation of the symptom) and into the message (assembler and non-verbal machine language). Obviously, this does not preclude the validity of the clinical history (semeiotics), essentially built on a verbal language rooted in medical reality.
We are aware that our Linux Sapiens is perplexed and wondering:«... could the logic of Classical language help us to solve the poor Mary Poppins' dilemma?»
(You will see that much of medical thinking is based on the logic of Classical language but there are limits) |
- ↑ Tanaka E, Detamore MS, Mercuri LG, «Degenerative disorders of the temporomandibular joint: etiology, diagnosis, and treatment», in J Dent Res, 2008».
PMID:18362309
DOI:10.1177/154405910808700406 - ↑ Roberts WE, Stocum DL, «Part II: Temporomandibular Joint (TMJ)-Regeneration, Degeneration, and Adaptation», in Curr Osteoporos Rep, 2018».
PMID:29943316
DOI:10.1007/s11914-018-0462-8 - ↑ Lingzhi L, Huimin S, Han X, Lizhen W, «MRI assessment and histopathologic evaluation of subchondral bone remodeling in temporomandibular joint osteoarthritis: a retrospective study», in Oral Surg Oral Med Oral Pathol Oral Radiol, 2018».
PMID:30122441
DOI:10.1016/j.oooo.2018.05.047 - ↑ Sadegh-Zadeh Kazem, «Handbook of Analytic Philosophy of Medicine», Springer, 2012, Dordrecht».
ISBN: 978-94-007-2259-0
DOI:10.1007/978-94-007-2260-6 - ↑ Cambridge Dictionary online
- ↑ Blouw P, Eliasmith C, «Using Neural Networks to Generate Inferential Roles for Natural Language», in Front Psychol, 2018».
PMID:29387031
DOI:10.3389/fpsyg.2017.02335
This is an Open Access resource! - ↑ Green K, «Dummett: Philosophy of Language», 2001».
ISBN: 978-0-745-66672-3 - ↑ Wikipedia entry
- ↑ Porporatti AL, Bonjardim LR, Stuginski-Barbosa J, Bonfante EA, Costa YM, Rodrigues Conti PC, «Pain from Dental Implant Placement, Inflammatory Pulpitis Pain, and Neuropathic Pain Present Different Somatosensory Profiles», in J Oral Facial Pain Headache, 2017».
PMID:28118417
DOI:10.11607/ofph.1680 - ↑ Jääskeläinen SK, «Differential Diagnosis of Chronic Neuropathic Orofacial Pain: Role of Clinical Neurophysiology», in J Clin Neurophysiol, 2019».
PMID:31688325
DOI:10.1097/WNP.0000000000000583 - ↑ Schick F, «Ambiguity and Logic», Cambridge University Press, 2003».
ISBN: 9780521531719 - ↑ Teigen KH, «The language of uncertainty», in Acta Psychologica, 1988».
DOI:10.1016/0001-6918(88)90043-1 - ↑ Varzi AC, «Vagueness», Nature Publishing Group, 2003, London, UK».
ISBN: 9780470016190
DOI:10.1002/0470018860 - ↑ Codish S, Shiffman RN, «A model of ambiguity and vagueness in clinical practice guideline recommendations», in AMIA Annu Symp Proc, 2005».
PMID:16779019
This is an Open Access resource! - ↑ Kong A, Barnett GO, Mosteller F, Youtz C, «How medical professionals evaluate expressions of probability», in N Engl J Med, 1986».
PMID:3748081
DOI:10.1056/NEJM198609183151206 - ↑ Bemmel J, Musen MA, «A Handbook of Medical Informatics», Houten/Diegem, 1997, Bonn, D».
- ↑ Osservability
- ↑ Chen HF, «On stochastic observability and controllability», in Automatica, 1980».
- ↑ Controllability Gramian
- ↑ Powel ND, Morgansen KA, «Empirical Observability Gramian for Stochastic Observability of Nonlinear Systems», arXiv, 2006».
- ↑ Melzack R, «The McGill Pain Questionnaire: major properties and scoring methods», in Pain, 1975».
PMID:1235985
DOI:10.1016/0304-3959(75)90044-5 - ↑ Melzack R, «Phantom limbs and the concept of a neuromatrix», in Trends Neurosci».
PMID:1691874
DOI:10.1016/0166-2236(90)90179-e - ↑ Melzack R, «From the gate to the neuromatrix», in Pain, 1999».
DOI:10.1016/s0304-3959(99)00145-1 - ↑ Melzack R, Wall PD, «On the nature of cutaneous sensory mechanisms», in Brain, 1962».
PMID:14472486
DOI:10.1093/brain/85.2.331 - ↑ Melzack R, Wall PD, «Pain mechanisms: a new theory», in Science, 1965».
PMID:5320816
DOI:10.1126/science.150.3699.971 - ↑ Petersen C, Malenka RC, Nicoll RA, Hopfield JJ, «All-or-none potentiation at CA3-CA1 synapses», in Proc Natl Acad Sci USA, 1998».
PMID:9539807 - PMCID:PMC22559
DOI:10.1073/pnas.95.8.4732 - ↑ Mouth of truth in Wikipedia
- ↑ Vanstone M, Monteiro S, Colvin E, Norman G, Sherbino F, Sibbald M, Dore K, Peters A, «Experienced Physician Descriptions of Intuition in Clinical Reasoning: A Typology», in Diagnosis (Berl), De Gruyter, 2019».
PMID:30877781
DOI:10.1515/dx-2018-0069 - ↑ 29.0 29.1 Stanley DE, Campos DG, «The Logic of Medical Diagnosis», in Perspect Biol Med, Johns Hopkins University Press, 2013».
ISSN: 1529-8795
PMID:23974509
DOI:10.1353/pbm.2013.0019 - ↑ Leape LL, Berwick DM, Bates DW, «What Practices Will Most Improve Safety? Evidence-based Medicine Meets Patient Safety», in JAMA, 2002».
PMID:12132984
DOI:10.1001/jama.288.4.501 - ↑ Graber ML, Wachter RM, Cassel CK, «Bringing Diagnosis Into the Quality and Safety Equations», in JAMA, 2012».
PMID:23011708
DOI:10.1001/2012.jama.11913 - ↑ Wikipedia article on Charles Sanders Peirce
- ↑ 33.0 33.1 Croskerry P, «Adaptive Expertise in Medical Decision Making», in Med Teach, 2018».
PMID:30033794
DOI:10.1080/0142159X.2018.1484898
particularly focusing on the field of the neurophysiology of the masticatory system